What Are Virtual Reality and Alternative Modalities for Burn Pain Management?
Virtual Reality and Alternative Modalities represent non-pharmacological approaches to managing pain in adult burn patients, with VR serving as the most extensively researched intervention. These methods use immersive technology and complementary therapies to interrupt pain signals and reduce the need for traditional pain medications.
VR for burn pain involves patients wearing head-mounted displays that transport them into interactive digital environments—typically peaceful nature scenes—during painful procedures like wound cleaning, dressing changes, and physical therapy sessions. The immersive experience engages multiple senses simultaneously, creating what researchers call “cognitive distraction” that competes with pain signals for the brain’s attention.
Alternative modalities that complement or combine with VR include:
- Guided imagery and meditation delivered through VR platforms
- Music therapy integrated into immersive environments
- Breathing exercises synchronized with virtual scenes
- Biofeedback displayed within VR interfaces
- Progressive muscle relaxation guided by virtual coaches
The technology has evolved significantly. As of February 2026, burn centers are using both active VR (where patients interact with the environment) and passive VR (where patients simply observe calming scenes) depending on the patient’s physical capabilities and treatment phase[6].
Choose VR-based approaches if: The patient is alert, able to wear a headset safely, and undergoing procedures lasting 10-45 minutes. Avoid if the patient has severe facial burns preventing headset use, active nausea, or significant cognitive impairment that prevents engagement.
How Does Virtual Reality Reduce Pain in Burn Patients?
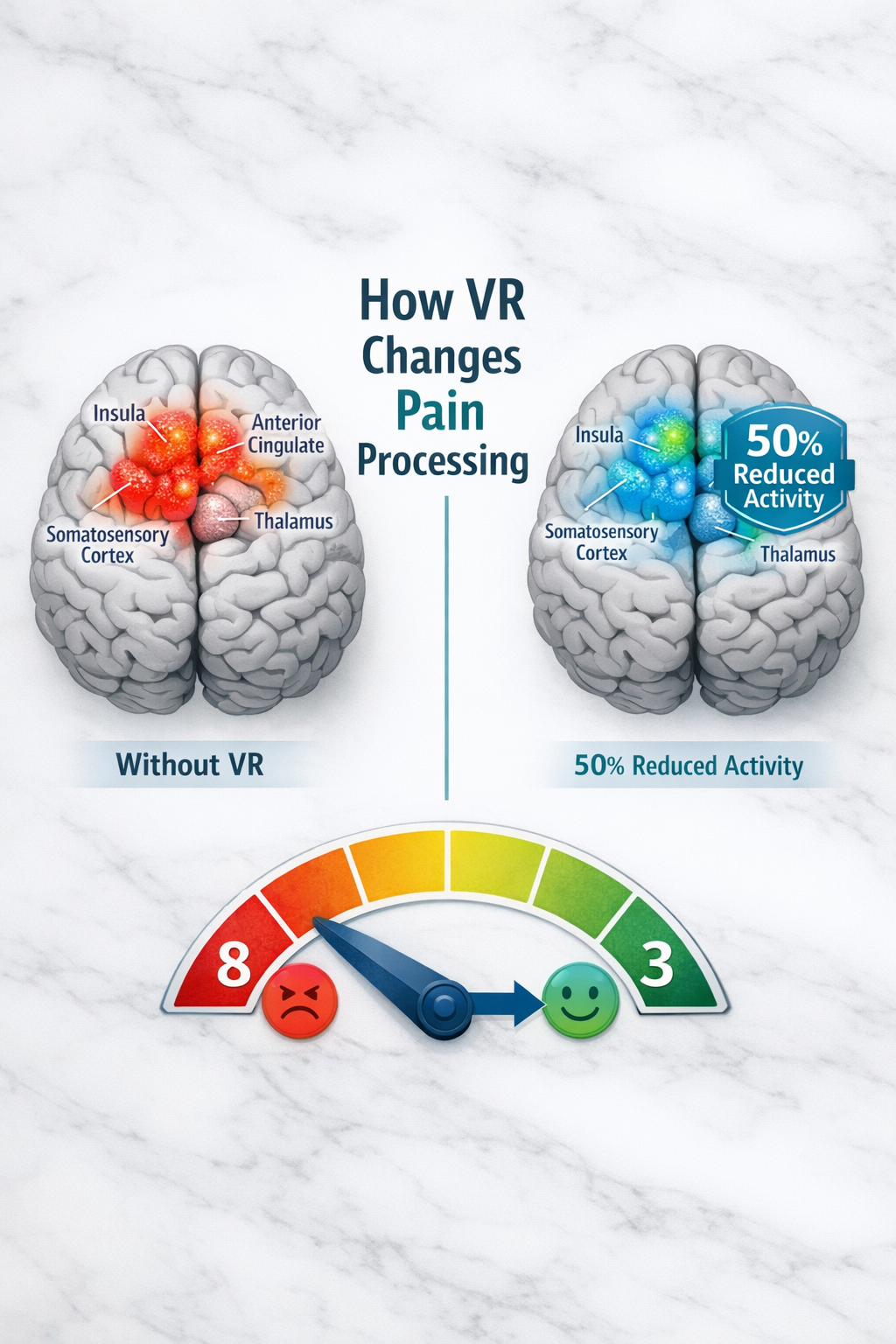
VR reduces pain through neurological mechanisms that fundamentally change how the brain processes pain signals. When burn patients use VR during painful episodes, brain imaging shows more than 50% reduction in activity in key pain-processing regions including the insula, anterior cingulate cortex, thalamus, and somatosensory cortices[2].
The Pain Gate Theory in Practice
VR operates on the gate control theory of pain, which proposes that the nervous system can only process a limited amount of sensory information at once. The immersive, multisensory VR experience floods the brain with competing visual, auditory, and sometimes haptic input, effectively “closing the gate” on pain signals trying to reach conscious awareness.
Measurable Brain Changes
The neurological impact is substantial and measurable:
- Reduced pain perception: Decreased activity in the anterior cingulate cortex (the emotional component of pain)
- Lower sensory processing: Diminished signals in somatosensory cortices (where physical pain is registered)
- Decreased threat response: Less activation in the insula (which processes pain’s unpleasantness)
A systematic review and meta-analysis of 11 randomized controlled trials involving 936 participants demonstrated a statistically significant overall effect with a moderate-to-large effect size (g = −1.528; 95% CI: −2.259 to −0.797; p < 0.001)[2].
Common mistake: Assuming VR simply “distracts” patients in a superficial way. The mechanism goes deeper—it actually alters pain processing at the neurological level, which is why effects can persist even after the headset is removed.
What Clinical Evidence Supports Virtual Reality and Alternative Modalities?
The clinical evidence for Virtual Reality and Alternative Modalities in burn care has reached a critical mass, with multiple high-quality studies published between 2024 and 2026 showing consistent benefits.
Key Research Findings
Saudi Arabia chest burn study (2024-2025): An active nature VR intervention with chest burn patients undergoing physiotherapy showed 79% pain intensity reduction in the VR group compared to 57% in the non-VR group (p < 0.001), with improvements sustained for 6 months post-treatment[1].
Integrative review results: Five of six quantitative studies and all three qualitative studies reported VR benefits for adult burn patients, with most supporting VR implementation as an effective pain management strategy[1].
Meta-analysis confirmation: The 2024 systematic review provided the strongest evidence yet, pooling data from 11 RCTs and confirming VR’s effectiveness across diverse wound types including burns, surgical wounds, and limb injuries[2].
Procedure-Specific Benefits
| Procedure Type | VR Benefit | Evidence Level |
|---|---|---|
| Wound dressing changes | Shorter duration, less pain | Multiple RCTs[1] |
| Physical therapy | 79% pain reduction | RCT[1] |
| Hand rehabilitation | Improved outcomes | Clinical studies[1] |
| Pre-procedural anxiety | Significant reduction | Multiple studies[1] |
Pediatric Population Shows Particular Effectiveness
While this article focuses on adults, it’s worth noting that the meta-analysis highlighted VR proved highly effective in pediatric populations specifically, where the distraction through immersive and multisensory environments generates particularly strong analgesic effects[2]. This suggests age-appropriate modifications could enhance adult outcomes.
Edge case: Some patients with pre-existing motion sensitivity or cybersickness may not tolerate VR well. Starting with shorter sessions (5-10 minutes) and static environments can help identify tolerance before longer therapeutic sessions.
How Are Hospitals Implementing VR Programs in 2026?
Major burn centers across the United States have expanded their Virtual Reality and Alternative Modalities programs significantly in 2026, moving VR from experimental to standard-of-care protocols.
The Clark Burn Center Model
In January 2026, Upstate Medical University’s Clark Burn Center launched an expanded VR program designed to help burn patients manage pain, limit painkiller use, and improve therapy outcomes[4]. Tamara Roberts, RN, Burn Program Manager, documented in February 2026 how VR devices are being actively integrated into physical and occupational therapy protocols[6].
Implementation Components
Equipment setup:
- Head-mounted displays (typically Meta Quest or similar devices)
- Sanitizable covers for infection control
- Content libraries featuring nature environments
- Adjustable straps for patients with facial injuries
Protocol integration:
- VR offered before painful procedures to reduce anticipatory anxiety
- Active use during wound care and dressing changes
- Integration into physical therapy sessions for range-of-motion exercises
- Post-procedure use for relaxation and recovery
Staff training requirements:
- Nurses trained in headset operation and troubleshooting
- Therapists certified in selecting appropriate VR content
- Protocols for identifying contraindications
- Documentation standards for tracking outcomes
Opioid Reduction Goals
The expanded programs specifically target opioid use reduction. VR application enables better pain management while reducing reliance on opioid medications, addressing concerns about pharmacological side effects and dependency[2]. This aligns with broader healthcare initiatives to combat the opioid crisis while maintaining effective pain control.
Choose active VR if: The patient can safely interact with controllers and benefits from engagement (e.g., during physical therapy). Choose passive VR if the patient needs to remain still or has limited hand function.
What Types of VR Content Work Best for Burn Patients?
The content delivered through Virtual Reality and Alternative Modalities significantly impacts therapeutic outcomes. Research has identified specific environment types and interaction patterns that optimize pain relief for burn patients.
Nature-Based Environments Dominate
Reviewed studies identified both active and passive VR scenarios, with natural environments serving as the primary therapeutic setting in most protocols[1]. These include:
Water scenes:
- Floating down calm rivers
- Underwater coral reef exploration
- Lakeside meditation environments
- Ocean wave observation
Forest environments:
- Walking through peaceful woods
- Mountain meadow experiences
- Autumn leaf scenes
- Redwood forest immersion
Sky and space themes:
- Cloud floating experiences
- Northern lights observation
- Gentle space exploration
- Sunrise/sunset scenarios
Active vs. Passive Content
Passive VR involves patients observing calming scenes without interaction. This works well during wound care when patients must remain still and cannot use hand controllers.
Active VR engages patients in simple interactions like picking virtual flowers, feeding virtual animals, or navigating paths. This approach proves particularly effective during physical therapy, where movement is therapeutic and the VR content can gamify rehabilitation exercises.
Duration and Timing Considerations
- Short procedures (10-20 minutes): Single immersive environment
- Longer procedures (20-45 minutes): Multiple scenes or progressive narratives
- Pre-procedural use: 5-10 minutes to reduce anticipatory anxiety
- Post-procedural use: 10-15 minutes for relaxation and recovery
Common mistake: Selecting overly stimulating or fast-paced content. Burn patients benefit most from calm, predictable environments that promote relaxation rather than excitement. Avoid action games, rapid scene changes, or content that could increase heart rate and anxiety.
Who Benefits Most from Virtual Reality and Alternative Modalities?
Virtual Reality and Alternative Modalities prove most effective for specific patient populations and clinical scenarios within burn care. Understanding these factors helps clinicians identify ideal candidates.
Ideal Candidates
Patient characteristics:
- Alert and oriented adults (18+ years)
- Moderate to severe pain during procedures (pain scores 4-10/10)
- Undergoing repeated painful procedures (dressing changes, debridement, therapy)
- Concerned about opioid use or experiencing medication side effects
- Open to technology-based interventions
Clinical scenarios:
- Chest burns requiring physiotherapy (79% pain reduction demonstrated)[1]
- Hand burns during rehabilitation exercises
- Partial-thickness burns during dressing changes
- Pre-procedural anxiety management
- Patients requiring opioid reduction strategies
Contraindications and Limitations
Avoid VR if the patient has:
- Severe facial burns preventing headset placement
- Active nausea or vomiting
- Severe claustrophobia triggered by headsets
- Significant cognitive impairment preventing engagement
- Seizure disorders triggered by visual stimuli
- Severe motion sickness history
Relative contraindications:
- Neck injuries limiting head movement
- Severe eye injuries or recent eye surgery
- Extreme agitation or confusion
- Inability to communicate discomfort
Special Populations
Older adults: May require additional orientation and simpler interfaces, but studies show effectiveness across age groups when properly introduced.
Non-English speakers: Visual nature-based content works well across language barriers, though interactive content may require language-appropriate versions.
Technology-averse patients: Brief demonstrations and gradual introduction (starting with 5-minute sessions) improve acceptance rates significantly.
Decision rule: If a patient can safely wear the headset, understands basic instructions, and experiences pain during procedures, trial VR for at least 2-3 sessions before determining effectiveness. Individual response varies, and some patients require adjustment periods.
What Are the Practical Challenges and Solutions?
Implementing Virtual Reality and Alternative Modalities in burn units presents practical challenges that healthcare teams must address for successful program adoption.
Infection Control Concerns
Challenge: VR headsets contact patient faces and hair, creating infection transmission risks in immunocompromised burn patients.
Solutions:
- Disposable sanitary covers for each patient
- Hospital-grade disinfection protocols between uses
- Dedicated devices for isolation patients
- UV sterilization systems for equipment
Equipment Costs and Maintenance
Challenge: Initial investment and ongoing maintenance costs can strain budgets.
Solutions:
- Grant funding from pain management foundations
- Demonstrating opioid cost savings to justify investment
- Starting with 2-3 devices to establish proof of concept
- Partnering with VR companies for pilot programs
Staff Training and Adoption
Challenge: Busy nursing staff may view VR as additional burden rather than time-saver.
Solutions:
- Emphasizing that VR can shorten procedure times[1]
- Providing hands-on training during non-critical times
- Designating VR champions among staff
- Tracking and sharing success metrics
Patient Acceptance Variability
Challenge: Not all patients embrace VR technology, particularly older adults or those unfamiliar with gaming.
Solutions:
- Offering demonstrations before painful procedures
- Starting with simple, calming content
- Allowing family members to try equipment first
- Respecting patient preferences without pressure
Technical Troubleshooting
Challenge: Equipment malfunctions during critical procedures can disrupt care.
Solutions:
- Maintaining backup devices
- Creating quick-reference troubleshooting guides
- Establishing IT support protocols
- Training multiple staff members on basic fixes
Edge case: Patients with claustrophobia may tolerate VR better with “pass-through” modes that allow them to see the real environment mixed with virtual elements, or with audio-only guided imagery as an alternative modality.
Conclusion
Virtual Reality and Alternative Modalities have transitioned from experimental interventions to evidence-based tools for pain management in adult burn patients. With documented pain reductions up to 79%, measurable changes in brain activity exceeding 50%, and growing implementation in major burn centers throughout 2026, VR represents a significant advancement in non-pharmacological pain control.
The clinical evidence is compelling: meta-analyses confirm moderate-to-large effect sizes, patients experience shorter procedures, anxiety decreases, and opioid requirements diminish. As healthcare systems prioritize both patient experience and opioid reduction, Virtual Reality and Alternative Modalities offer a practical solution that addresses both goals simultaneously.
Actionable Next Steps
For healthcare administrators:
- Research grant opportunities for VR equipment acquisition
- Calculate potential opioid cost savings to justify investment
- Contact burn centers with established programs (like Upstate Medical University’s Clark Burn Center) for implementation guidance
For burn unit clinicians:
- Identify 2-3 patients who could benefit from VR trials
- Attend training sessions on VR equipment operation
- Document pain scores before and after VR use to build internal evidence
For burn patients and families:
- Ask your care team if VR is available at your facility
- Request a demonstration before painful procedures
- Communicate openly about your experience to help optimize the approach
For researchers:
- Investigate optimal VR content types for specific burn locations
- Study long-term outcomes and sustained pain reduction
- Explore combination approaches with other alternative modalities
The future of burn pain management increasingly includes immersive technology alongside traditional approaches. As equipment becomes more affordable and evidence continues mounting, Virtual Reality and Alternative Modalities will likely become standard offerings in comprehensive burn care programs.
Frequently Asked Questions
Does VR completely eliminate pain during burn procedures?
No, VR significantly reduces pain but doesn’t eliminate it entirely. Studies show 79% reduction in pain intensity, meaning patients still experience some discomfort but at much more manageable levels that require less medication[1].
How long do the pain-reducing effects of VR last?
Pain reduction is strongest during VR use, but studies show benefits can persist for hours after removal. One study documented sustained improvements for 6 months post-treatment when VR was used regularly during therapy[1].
Can VR replace pain medications entirely?
VR should complement, not replace, pain medications. It allows for reduced opioid doses while maintaining effective pain control, but most patients still need some pharmacological support for severe burn pain.
What if a patient gets motion sickness from VR?
Start with static environments and shorter sessions (5-10 minutes). If motion sickness persists, alternative modalities like audio-guided imagery or music therapy can provide similar distraction benefits without visual immersion.
Is VR safe for patients with facial burns?
It depends on burn location and severity. Patients with facial burns may not tolerate headset pressure, but some devices offer adjustable straps that avoid burned areas. Clinicians assess safety case-by-case[6].
How much does VR equipment cost for a burn unit?
Consumer-grade VR headsets suitable for medical use range from $300-$500 per device. A complete program including 3-5 devices, sanitation equipment, and content licenses typically costs $3,000-$8,000 initially.
Do insurance companies cover VR therapy for burn patients?
Coverage varies by insurer and region. As of 2026, some insurers recognize VR as a covered pain management modality, but many still consider it experimental. Hospitals often absorb costs as part of comprehensive burn care.
What age groups benefit most from VR pain management?
Research shows effectiveness across age groups, though pediatric populations show particularly strong responses. Adults of all ages benefit when properly introduced to the technology[2].
Can VR be used during skin grafting procedures?
VR is most commonly used during wound care, dressing changes, and physical therapy rather than surgical procedures requiring anesthesia. However, it may reduce pre-operative anxiety before grafting procedures.
How quickly do patients adapt to using VR?
Most patients adapt within one 10-15 minute session. Some technology-averse patients may need 2-3 exposures to feel comfortable, but the intuitive nature of modern VR interfaces facilitates quick adoption.
Does VR work for chronic pain after burns heal?
Research primarily focuses on acute procedural pain, but emerging evidence suggests VR may help manage chronic neuropathic pain and phantom sensations after burn healing. More research is needed in this area.
What happens if VR equipment malfunctions during a procedure?
Burn units with VR programs maintain backup devices and can quickly switch to traditional pain management if needed. Staff training includes contingency protocols for technical failures.
References
[1] Virtual reality as an intervention for adult burn patients – https://pmc.ncbi.nlm.nih.gov/articles/PMC11924071/
[2] Virtual reality as a pain reduction method in burn and wound healing – https://pmc.ncbi.nlm.nih.gov/articles/PMC12888808/
[4] VR Burn Program – https://www.upstate.edu/news/articles/2026/2026-01-22-vrburn.php
[6] Virtual Reality Devices for Burn Treatment – https://www.youtube.com/watch?v=lc0AaV5NsV8